Health Security Support in the Middle East and North Africa
Overview
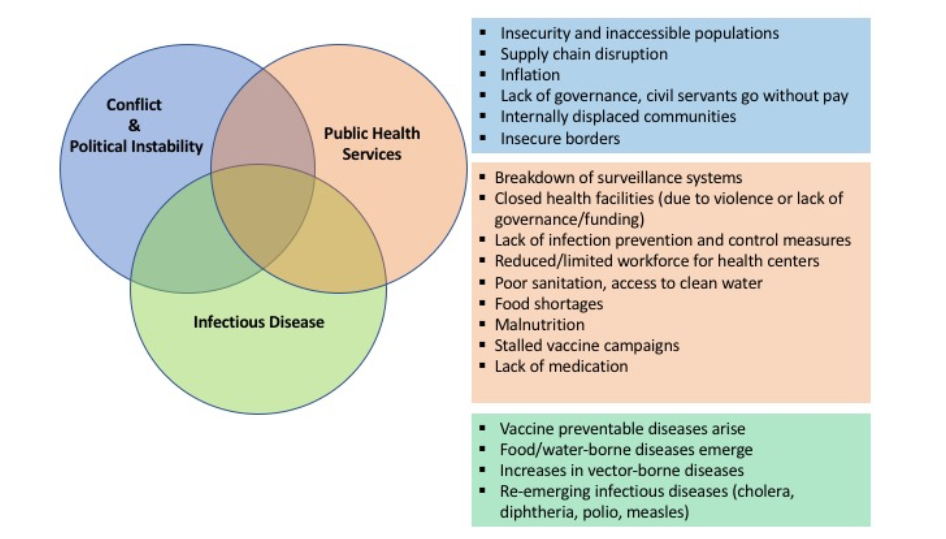
The influence of political instability and conflict on the emergence and spread of infectious diseases during humanitarian crises has been evident in recent years. For example, the devastating cholera outbreak first reported in Yemen in 2016 can be directly linked to Saudi airstrikes on civilian power and water infrastructure, and was exacerbated by existing strains on the population and health system, such as wide-spread starvation and malnutrition, destruction of primary health care centers, and lack of medical supplies and personnel. The disruption of routine vaccination services in Syria, due to the civil war on-going since 2011, resulted in re-emergence of wildtype poliovirus in 2013, later declared a Public Health Emergency of International Concern by the WHO in 2014. Our team at the Center for Global Health Science and Security at Georgetown University is interested in operational and implementation research questions related to sustainable health systems strengthening, with an emphasis on the prevention, management, and control of infectious diseases in humanitarian situations, and particularly countries and regions affected by conflict.
Health Security Support for Libya
Libya faces perennial challenges of sustaining health security capabilities alongside civil unrest, political instability, and terrorism. In situations like Libya’s, there is a need for creative, flexible and innovative implementation approaches when it comes to health systems strengthening. We are partnering with the Libyan National Centre for Disease Control (NCDC) and the National Centre for Animal Health (NCAH) on two distinct projects.
The first is to develop laboratory capacity across key public health and veterinary laboratories to improve biorisk assessments and policies as well as waste management practices. Our team is collaborating with the Princess Haya Biotechnology Center at Jordan University of Science and Technology to develop assessment tools that can be applied across Libyan laboratories for a holistic and sustainable approach.
Our second project focuses on mapping existing capacities for rapid detection and response for priority zoonoses in order to develop regional One Health Rapid Response Teams (OH-RRTs). These projects prevent duplication across NCDC and NCAH and allow for improved capacity and expanded geographical range to detect priority zoonotic diseases and work under safe laboratory environments in high risk, high threat areas of Libya.

Morocco Laboratory Assessment
Building on from work in Libya, in December 2018 we were awarded funding from the U.S. Department of State to adapt an existing laboratory assessment tool for application in Morocco. The number of clinical, diagnostic, and research laboratories is rising rapidly in Morocco, especially in the private sector, yet there are concerns that these facilities lack the necessary infrastructure, equipment, and training to safely and securely handle specimens that may contain dangerous pathogens. In particular, systems for sample inventory and storage are not routinely in place. Our project, implemented in collaboration with laboratory biosafety experts from the Eastern Mediterranean Public Health Network, will work with laboratories in Morocco to assess and improve biorisk management, with an emphasis on safe and secure inventory.
Developing methodologies to support Joint External Evaluations (JEE) in crisis countries
The ability to deal with a catastrophic public health event relies on strong health infrastructure and robust collaboration across sectors. The risk of a national event becoming a global concern is amplified when national capacities to detect, report, and respond to a potential pandemic are obstructed by political instability and conflict. With support from the Open Philanthropy Project, we are reviewing current mechanisms in place for implementing the JEE in WHO designated crisis countries. We plan to establish a “crisis methodology” that will allow for a robust, evidence-based review to identify critical gaps and develop a clear action plan that can be validated by key stakeholders, adapted post-conflict, and may be used for countries in crisis.
Publications
Georgetown Center for Global Health Science and Security. Establishing Infectious Disease Research Priorities in Areas Affected by Conflict. Report funded by the Georgetown University Global Health Initiative. May 2018.
Sorrell E., Standley CJ. (2018). Infected by Conflict. APPS Policy Forum.